Usutu
This is an extremely rare avian infection in humans, which originates from Africa. It takes its name from a south African river (the Great Usutu or Maputo river), which flows near a small village in Natal where the virus was first isolated in a female Culex neavei mosquito.
CAUSATIVE AGENT AND INFECTIVE CYCLE
As with West Nile fever, the causative agent is a bird pathogenic Flavivirus. The two viruses differ when it comes to the rate of mortality in birds (high in the case of USUV, low in the WNV), and with the impact it has on public health (the WNV is responsible for numerous human cases with severe neurological symptoms; the USUV has so far been found in a few minor cases).
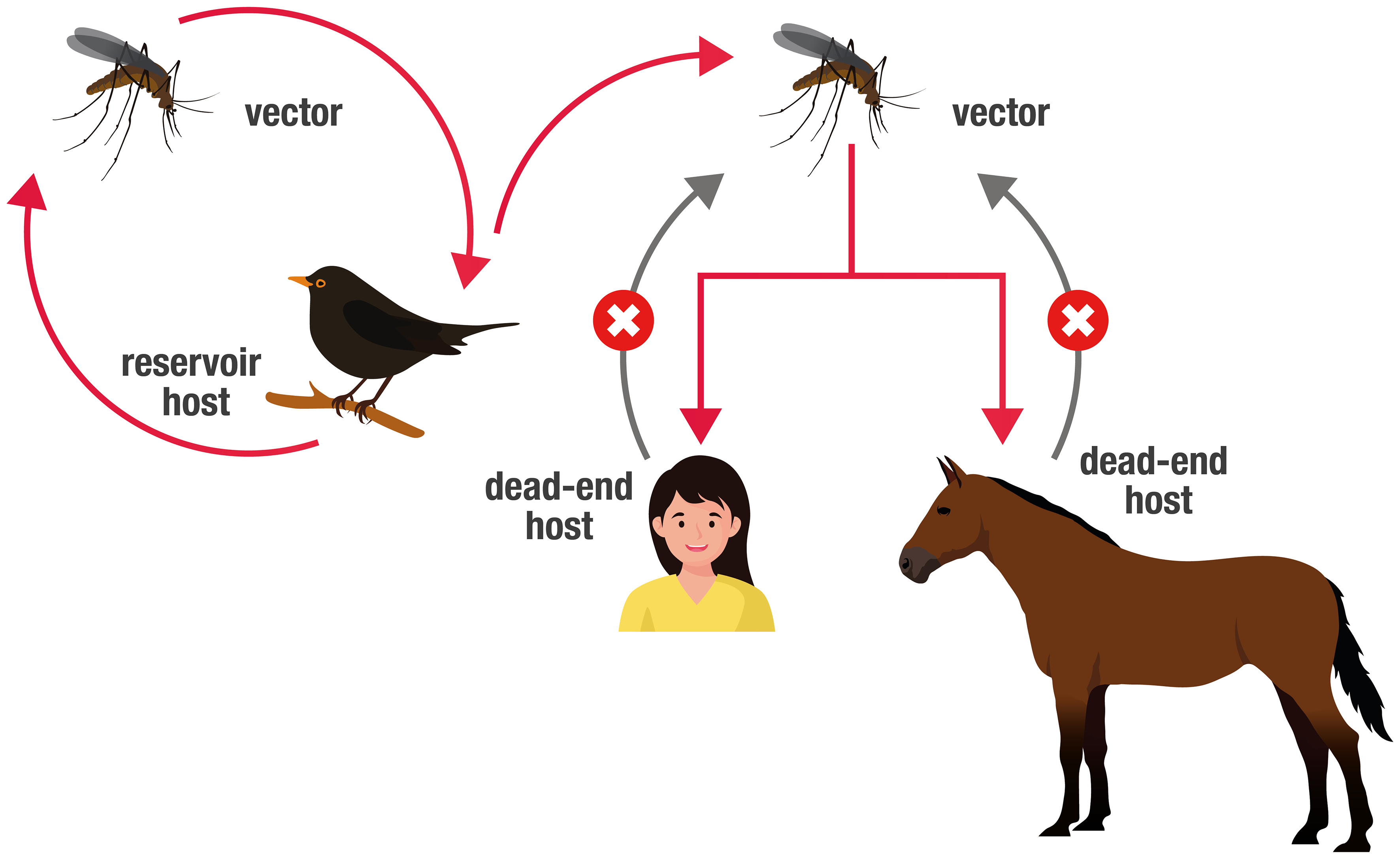
Poultry farming species appear to be resistant to infection, as are wild African species. However, among European birds, mortalities have been found in many species, especially in passerines (blackbirds, house sparrows, blue tits, great tits, nuthatches, robins, and song thrushes), but also in the order Strigiformes. Migratory birds played a key role in the spread of the virus out of Africa.
The vector responsible for the infection is the ornithophilous mosquito. In Europe, it has been mainly isolated in Culex pipiens, but also in Aedes albopictus, Ae. vexans, Ae. rossicus, Anopheles maculipennis, Ochlerotatus caspius, Oc. detritus, Cx. hortensis, Cx. territans, Cx. perexiguus and Culiseta annulata. However, only the Cx. pipiens (in Europe) and the Cx. neavei (in Africa) have so far been confirmed as competent vectors of the virus.
Mammals including humans, can be random and dead-end hosts. Transfusion of blood or derivatives and transplantation of infected tissues and organs can also be other causes of infection.
SYMPTOMS AND COURSE OF THE DISEASE
In humans, there has not been a lot of information with regards to USUV infections. In Africa, only two isolations in human beings are known so far, almost nothing is known about their clinical symptoms. In the first case (an adult in the Central African Republic in 1981), the patient demonstrated symptoms of fever and a skin rash; in the second case (a child in Burkina Faso in 2004), fever and jaundice.
In Europe, a greater number of cases are known and are all recent. The oldest date back to 2009 in Italy (Emilia Romagna) and are associated with the onset of neurological disorders in two immunocompromised patients, both survived. One patient developed a fever and neurological symptoms following chemotherapy treatment for B-cell lymphoma. The other patient developed thrombotic thrombocytopenic purpura, a fever, and hepatitis after a trip to Egypt; subsequent rapid and progressive development of neurological symptoms followed, which led to a coma. The hepatitis patient necessitated a transplant. Both patients received plasma transfusions during treatment, but it is unclear whether the virus was acquired naturally or through transfusions.
Subsequently, the USUV genome was isolated in the cerebrospinal fluid of patients with suspected meningoencephalitis in Italy and in a patient with a skin rash in Austria.
The presence of anti-USUV antibodies has been confirmed in asymptomatic blood donors in Italy, Germany and in patients with clinical symptoms in Croatia concurrent with the WNV infection. The presence of mild symptoms (fever, rash, jaundice, headache, neck stiffness, hand tremors and hyperreflexia) that are easily confused with those of other diseases, certainly leads to an underestimation of the number of human cases.
A retrospective study carried out on almost a thousand serum and cerebrospinal fluid samples collected in the Modena area between 2008 and 2011, has shown that human infection is not so infrequent and even more widespread than that of WNV. In horses, seroconversion has been observed in various parts of Europe, but these animals appear not to be susceptible to the disease.
TREATMENT AND PREVENTION
There is currently no specific therapy or vaccination for USUV.
Prevention consists in protecting yourself from bites and preventing mosquitoes from reproducing easily.
Therefore, it is advisable to:
- use repellents and wear long trousers and long-sleeved shirts when outdoors;
- use mosquito nets on the windows;
- frequently empty flowerpots or other containers (e.g., buckets) with stagnant water;
- change water bowls for animals frequently;
- keep paddling pools in an upright position when not in use.
For further information about prevention please click here!
Last modified: Jan 2021



